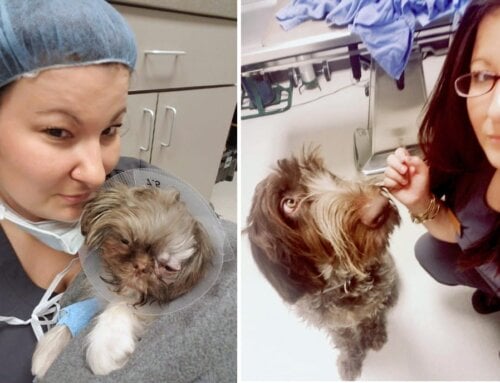
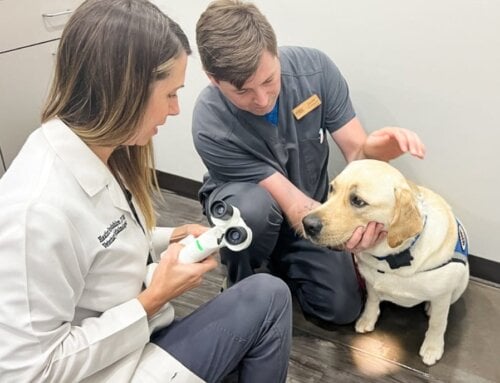
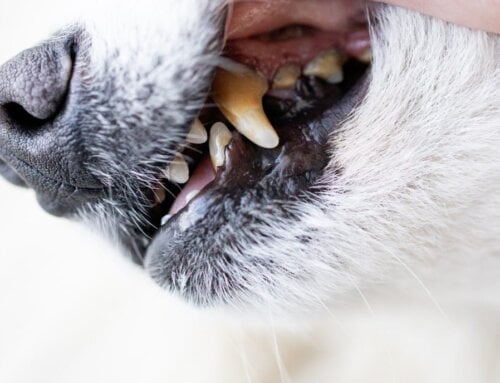
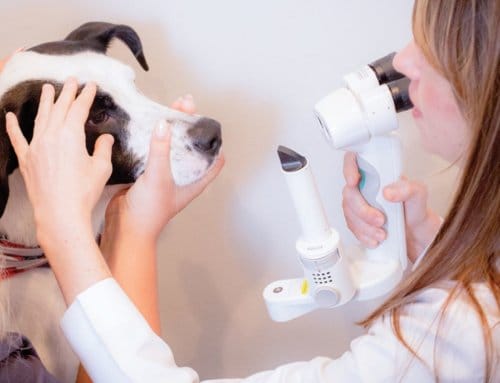
Uveitis is an ocular condition that occurs when the uveal tract within the eye becomes inflamed, which can lead to alterations in vision, intraocular pressure and comfort. Read on for common clinical signs, how we test for the condition, causes, and treatment options.
Uveitis is inflammation of the uveal tract, the vascular tissue within the eye. This tissue plays many roles in the overall health of the eye. It provides nutrients to ocular structures, helps regulate intraocular pressure, supports the important barrier between the blood and the eye, maintains clarity of the fluid within the eye and supplies nutrition to the retina (an important structure for vision). Disorders of the uvea often lead to alterations in vision, intraocular pressure and comfort.
The simplified anatomy of the eye can be divided into 3 layers: an outer fibrous layer consisting of the cornea and sclera, a middle vascular layer consisting of the choroid, iris and ciliary body (aka the uvea or uveal tract), and an inner neurological layer consisting of the retina and optic nerve. Uveitis is therefore simply inflammation within the uveal tract, or vascular layer within the eye.
The uveal tract is composed of three parts:
- Iris, or colored part of the eye
- Ciliary body, located just behind the iris, which forms the fluid within the eye
- Choroid, located in the back of the eye behind the retina
The specific pathophysiology of uveitis depends on the underlying cause, but in all cases, there is a breakdown of the blood-eye barrier that normally keeps cells and large proteins from entering the eye. When the uveal tract becomes inflamed, white blood cells can enter the eye and cause damage to the eye. Uveitis can be broken down further by whether it affects the front portion of the eye (iris and ciliary body; Anterior Uveitis), back of the eye (choroid; Posterior Uveitis), or all of the eye (Panuveitis).
Common clinical signs of uveitis include: squinting, tearing, red eye, cloudy cornea, hazy anterior chamber, blood or white blood cells in the bottom of the eye, change in iris color or shape, swollen iris, small pupil and decreased vision.
When uveitis is suspected, the following clinical tests are recommended:
Complete physical and ocular exam:
- Slit-lamp exam, to look for aqueous “flare,” a hallmark sign.
- Fundus exam, to look for evidence of vision-threatening posterior uveitis.
- Tonometry, to measure intraocular pressure.
- Fluorescein stain, to rule out a corneal ulcer.
Labwork considerations:
- Complete blood count (CBC), biochemistry panel and urinalysis.
- Infectious disease testing panels, appropriate to patient history and species.
Imaging considerations:
- Chest X-rays and abdominal ultrasound, to look for evidence of cancer or infection in the body.
It can be difficult to determine the cause of uveitis. Determining one, however, is necessary due to the potential threat to vision or the possibility of a more significant systemic disease.
The top three causes of uveitis fall into the broad categories of infectious, immunemediated, and neoplastic disease, however uveitis can also occur secondary to disease of the lens, or other metabolic, vascular, traumatic, toxic, or reflexive causes.
Common causes of uveitis in dogs and cats include auto-immune issues, trauma, high blood pressure, cataract formation, or secondary to systemic infection or cancer. It also may occur secondary to a corneal ulcer, known as reflex uveitis.
Finally, in approximately 50% of cases in dogs and cats, we are unable to find a specific underlying cause, and consider the uveitis to be idiopathic. This diagnosis is made by exclusion, meaning we have to rule out the other more serious causes first before reaching this diagnosis.
Anti-inflammatory corticosteroids and nonsteroidal medications are the primary therapy for uveitis. These include both topical eye drops and oral medications. Oral antibiotics may be started if an infection is suspected, or prophylactically. Other treatments considered include mydriatic/cycloplegic therapy (pupil dilator to help relax the muscle that causes the pupil to constrict), oral pain medications, and specific therapy based on the underlying cause.
We often recommend pet patients return for a pressure check within the first few days after diagnosis to make sure that glaucoma (high pressure within the eye) has not developed. If the patient is doing well at home, we suggest they return for a recheck every 1-2 weeks until the disease is in remission. Once the inflammation is controlled, we gradually reduce the medical therapy and continue to closely monitor the pet for any signs of a relapse.
It is important to monitor these cases closes closely, because in some cases, there may be complications to uveitis that may lead to glaucoma, permanent vision loss, retinal detachment or cataract formation. If monitored and treated appropriately, most cases of uveitis will be controllable, and pet patients will maintain their comfort and vision on a long-term basis.
Golden Retrievers can get a special type of heritable uveitis called pigmentary uveitis, or Golden Retriever uveitis.
We keep an eye out for this when examining breeding dogs.
Uvetis DDX:
- Infectious
- Bacterial
- Septicemia / endotoxemia
- Leptospira sp.
- Borrelia burgdorferi
- Brucella sp.
- Bartonella spp.
- Fungal
- Blastomyces sp.
- Histoplasma capsulatum
- Cryptococcus spp.
- Coccidioides immitis
- Aspergillus sp.
- Rickettsial
- Ehrlichia canis, Ehrlichia platys
- Rickettsia rickettsii
- Protozoal
- Toxoplasma gondii
- Leishmania donovani
- Parasitic
- Dirofilaria immitis
- Toxocara spp.
- Baylisascaris spp. (ocular larval migrans)
- Taenia multiceps
- Angiostrongylus vasorum
- Viral
- Canine adenovirus types 1 and 2 (immune-mediated)
- Canine distemper virus
- Canine herpesvirus 1
- Rabies virus
- Algal
- Prototheca spp
- Geotrichia spp.
- Bacterial
- Immune-mediated
- Immune-mediated vasculitis
- Immune-mediated thrombocytopenia
- Uveodermatologic syndrome (Vogt-Koyanagi-Harada-like syndrome)
- Inherited
- Pigmentary uveitis in the Golden Retriever
- Idiopathic
- Neoplastic / Paraneoplastic
- Lymphosarcoma
- Ciliary body adenocarcinoma
- Intraocular melanoma
- Hemangiosarcoma
- Other primary and metastatic neoplasms
- Granulomatous meningoencephalitis
- Lens-associated
- Cataract-induced (phacolytic; immune-mediated)
- Lens capsule rupture (phacoclastic; immune-mediated)
- Lens luxation
- Metabolic
- Diabetes mellitus (lens-induced)
- Hyperlipidemia
- Vascular
- Systemic hypertension
- Hyperviscosity syndrome
- Polycythemia
- Coagulopathy
- Periarteritis nodosa
- Trauma
- Blunt trauma
- Penetrating trauma
- Corneal foreign body
- Toxic
- Prostaglandin derivatives (latanoprost)
- Sulfamethazine-trimethoprim (immune-mediated)
- Reflex uveitis
- Keratitis
- Episcleritis
- Scleritis
Do you think your pet or pet patient should be seen for uveitis?
Please call us today at 757-749-4838.